Here we will explain how to prepare for scoliosis surgery, from preparation to hospitalization.
There are three types of imaging tests: x-ray, CT scan and MRI scan.
Taken from both front and side in a standing position, to examine the pattern and extent of the spinal curve.
Taken on your back to see how far the curve is reduced by traction on the limbs
Taken from on your side to see how far the rounded back is warped by putting a pillow in the back.
The shape and size of the vertebral arch and vertebral body are checked, as well as the vertebral root where the screw is inserted. The CT values are measured to determine bone strength.
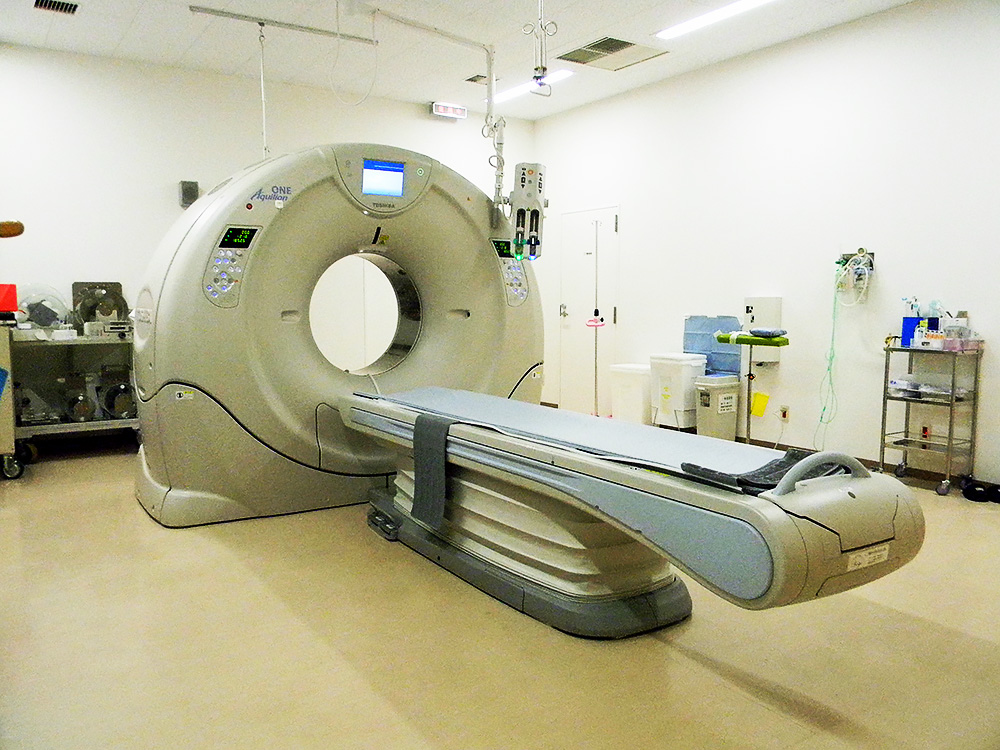
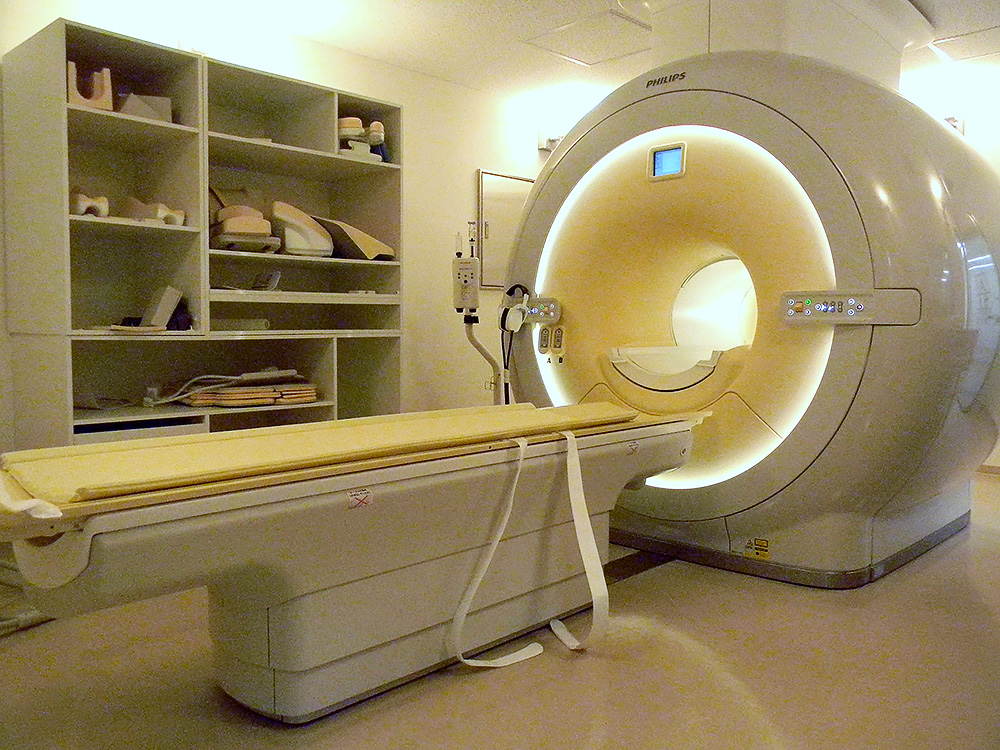
Check for spinal cord, caudal nerve and nerve root stenosis, as well as for syringomyelia.
Autologous blood banking is a pre-surgical preparation. This is because you may become anemic due to bleeding during or after surgery.
It is also possible to have a blood transfusion provided by the Japanese Red Cross Society. Younger patients to those in their 70s can store their own blood in advance and use it during and after surgery.
Autologous blood storage is started regularly about one month before the surgery, storing 600-1200 ml of blood for posterior corrective fixation and 400-800 ml of blood for anterior corrective fixation.
You may be unable to save blood due to underweight, anemia or complications, or unable to save much blood. If there is a lot of bleeding in that case, a Japanese Red Cross blood transfusion may be given. Blood loss during surgery is 200-800 ml (usually less than 1,000 ml) if it's small. In extremely rare cases, it may be as much as 2000ml.
EKG, echocardiogram, respiratory function test, blood test and urine test will be performed.
If the spinal curve is large and the breathing function is poor, deep breathing exercises are performed.
Adults and older patients will have their bone density and CT values measured, as well as bone metabolic markers (blood draw), and possibly one or two injections of bone strengthening prior to surgery.
This is not necessary for young patients.
The length of stay in the hospital is around 1 week to 10 days. For older patients, it can be up to 2 weeks. This is just a reference.


The next day, the patient will return to the general ward and we will change your position regularly. (To prevent bed sores, prevent atelectasis and pneumonia, and improve bowel movement.)
Intravenous antibiotics will be administered for four to five days after the surgery.
Meals will be started when you are able to pass gas. You can start drinking a little bit of fluid the day after surgery. In case the patient is unable to start eating for a long period of time, an intravenous drip will be administered.
You will be trained to walk in an upright position within 2-3 days of surgery (a rehabilitation therapist will be in charge).
The drain tube (which prevents blood from accumulating in the wound) will be removed 5-6 days after the surgery. In most patients, the pain subsides and the patient is able to walk on the third day after surgery (* exceptions may apply).
The pain is usually reduced on the third day after surgery and is almost completely gone in about a week (*exceptions may apply). Children and young patients in particular tend to get rid of the pain rapidly. The pain may last a little longer for older patients. Pain medication will be administered to control and manage the pain while it is present.
After discharge from the hospital, you will be asked to visit an outpatient clinic within a month for follow-up. The corset will be measured and made while you are in the hospital and you will wear it for 3 months from the date of surgery. Strong forward bending and heavy lifting should be avoided till 6months after the date of surgery.
You will be seen again at 3 and 6 months, and the next visit will be one year later. In most cases, after 6 months, the bone fusion is complete and the patient is free (*exceptions may apply). In the meantime, you will continue to lead a normal life.